 There’s a good short piece, Humans Have Ten Times More Bacteria Than Human Cells: How Do Microbial Communities Affect Human Health?, in Science Daily, picks up on some of the themes we discussed in The human ’super-organism.’ The overwhelming majority of cells in human bodies belongs to microbes — the article says 10 bacteria cells for every human body cell (does it make you feel tired to think how much bacteria you’re carrying around?). Recognizing that we are a shambling micro-cosmos of oraganisms (or ‘microbiome’) suggests new understandings of all sorts of things, including disease. The Science Daily article points out that ‘changes in these microbial communities may be responsible for digestive disorders, skin diseases, gum disease and even obesity.’
There’s a good short piece, Humans Have Ten Times More Bacteria Than Human Cells: How Do Microbial Communities Affect Human Health?, in Science Daily, picks up on some of the themes we discussed in The human ’super-organism.’ The overwhelming majority of cells in human bodies belongs to microbes — the article says 10 bacteria cells for every human body cell (does it make you feel tired to think how much bacteria you’re carrying around?). Recognizing that we are a shambling micro-cosmos of oraganisms (or ‘microbiome’) suggests new understandings of all sorts of things, including disease. The Science Daily article points out that ‘changes in these microbial communities may be responsible for digestive disorders, skin diseases, gum disease and even obesity.’
There’s one passage in particular that I thought was worth posting, even if I don’t have too much to add:
“This could be the basis of a whole new way of looking at disease. In order to understand how changes in normal bacterial populations affect or are affected by disease we first have to establish what normal is or if normal even exists,” says Margaret McFall Ngai of the University of Wisconsin, Madison.
The microbiome research is particularly interesting to us at Neuroanthropology, even though it’s not strictly about the brain or nervous system, because it’s a particular compelling demonstration that the human body is a dynamic system; that is, the body is a system of different forces and processes, at a number of scales, that together continually produce the whole, sometimes in equilibrium and sometimes in ways that produce dysfunction.
Studies of microbes on the skin have found that around 50% belong to ten species, but some bacteria are specific even to a single person: “What was interesting about some of the other species with smaller populations is that they were host specific. We could only identify them on a single host. It is entirely possible that everyone could have a unique bacterial signature,” says Martin Blaser of New York University. Blaser has gone on to study the epidermal microbiome of patients with psoriasis and found that they have distinctive bacterial populations (the article doesn’t even hazard to suggest whether these differences might be cause or effect of their skin conditions).
Recognizing its importance, the National Institutes of Health in December 2007 announced the Human Microbiome Project as part of its Roadmap for Medical Research, devoting over $100 million in grants over the next five years.
In particular, the research will target five regions of the body: the skin, mouth, gastro-intestinal tract, nose, and female urogenital system.
To my knowledge, there’s not really a focus on the idea that different human populations might support different microbial populations. The account in Science Daily seems to focus exclusively on the contrast between ‘normal’ and disordered or diseased. Although I heartily support the research, and just can’t wait to check out the cool results, I would simply echo Ngai’s caveat that we don’t know ‘if normal even exists.’ I’m betting, especially reading some of the material from Blaser about idiosyncratic species, that ‘normal’ is likely to be pretty hard to pin down.
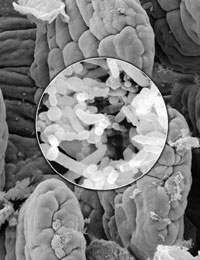
Photograph:
Scanning electron microscope images of B. thetaiotaomicron, human gut bacterium, and the intestine. Photo from PLoS Biology 2007 July; 5(7): e199. Published online 2007 June 19. doi: 10.1371/journal.pbio.0050199. Found at Baylor College of Medicine’s website.
Thanks to Bora Zivkovic at A Blog Around the Clock for putting me onto the original Science Daily article. Bora, you’re a blogging machine.
References
American Society for Microbiology. 2008 (June 5). Humans Have Ten Times More Bacteria Than Human Cells: How Do Microbial Communities Affect Human Health?. ScienceDaily. Retrieved June 7, 2008, from http://www.sciencedaily.com /releases/2008/06/080603085914.htm

This research is fascinating, Greg; I’m glad you posted on it. I particularly like your emphasis on the importance of variation; otherwise, whatever population is studied first gets classified as “normal”. And given the abundance and variety of bacteria, and the synergy between environments and people, there is likely to be a wide range of “normals”…
From an evolutionary perspective we would expect and hope for a wide range of “normals.” Since DNA is our genetic toolkit for adapting to life’s challenges, a wide range of time tested problem solvers is ideal. What is fascinating is the coevolution of us, bacteria, and our food. Bacteria can pick up, use, and discard DNA like tools, they alter our DNA and functionality, and make food more bio available. It is interesting that cultured foods are called cultures, considering they go back to probably the very beginning of culture, are passed on, and brought along migration routes. I would really like to know what anthropologists are looking at cultural practices and their influence on gut ecology. It seems the United States has a culture of mostly “dead” foods: pasteurized, sterilized, laden with preservatives. There is a growing appreciation for the importance of probiotics, however, they take the new form of a commodity to be produced, bought, and sold, rather than a culture that is individually crafted, maintained, and shared.
I’m just curious about what you said here, the part that goes
on what grounds could we assume the conscious ‘you’ in that sentence is distinct from the super-you aggregate? I’m just curious, and before you say, “neural correlates” I might offer that although the dash-board indicators show speed, oil pressure and fuel levels, it is in fact the alien unmechanical non-bus part of the vehicle that houses the intelligence if its conscious actions 😉
But I don’t want to be adversarial here, I just want to know: two days ago it was unthinkable that bathing in anti-bacterials was not a great idea, and here now today can we really discount that these creatures are entirely and delimitedly non-us?
No problem, Mr. G. I agree, who’s to know what the ‘you’ is if we are, in fact, super-organisms. I would say that it drives an even deeper wedge between the phenomenological ‘I’ (the one the reasons, feels, perceives) and this incredible super-organism that supports it, the vast majority of which is completely unavailable to that phenomenological ‘I.’ So, yes, talking about ‘you’ feeling tired is just a joke, but it shows up the irony.
For example, even our mitochondria, from a genetic perspective, are their own ‘thing’ (and were likely taken on board by very simple single- or multi-celled organisms a veeeeeery long time ago. Without them, and their distinctive DNA (not the same as our cell nuclei), we would be a hell of a lot more ‘tired’ (actually, we couldn’t function to produce energy, so we’d be a lot worse off).
No, I agree with you whole-heartedly; for so long, we’ve taken a kind of scorched-earth, kill-them-all-let-god-sort-them-out approach to microbial life, so much so that we’ve likely screwed with our environments and with the fauna that inhabit Us. We absolutely cannot delimit ourselves and say definitively, ‘this is where we stop. these other things living all over our skins are not part of us,’ because, from a functional viewpoint, we don’t work without them.
It’s a great point you make though, and one I didn’t bring up, which is the way that this should shift our understanding of how we treat microbial life in relation to our own health. Many of us were already getting squeamish about all the anti-bacterial stuff out there — this new research should make us even more reluctant to dump chemicals on ourselves that might turn out to be the microbiome version of DDT. Good point, Mr. G.